Theįracture site was subsequently debrided and the persistent physeal cartilage was The fracture extended through a persistent olecranon physis because of rounded bonyĮdges, smooth cartilage in place of cancellous intramedullary bone, and fracturedĬartilage at the joint surface, suggesting preinjury physeal deformity and nonunion. On visualization of the fracture site, it was apparent that Full-thickness flaps were developedĭown to the fracture site. A posterior approach was utilized, with a longitudinalĬurvilinear incision centered over the olecranon. 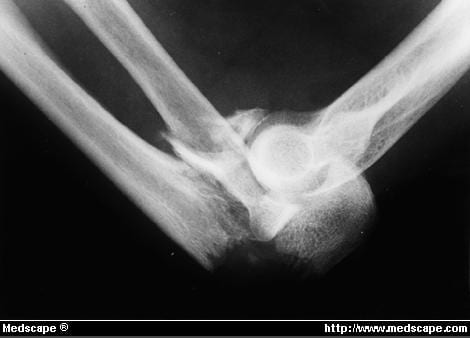 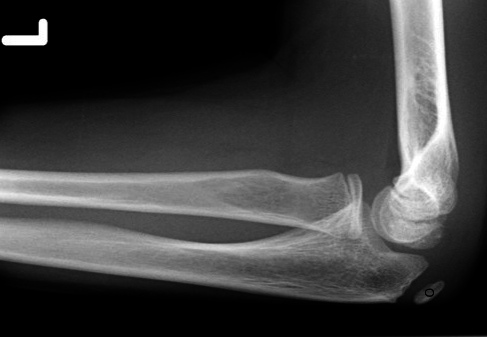
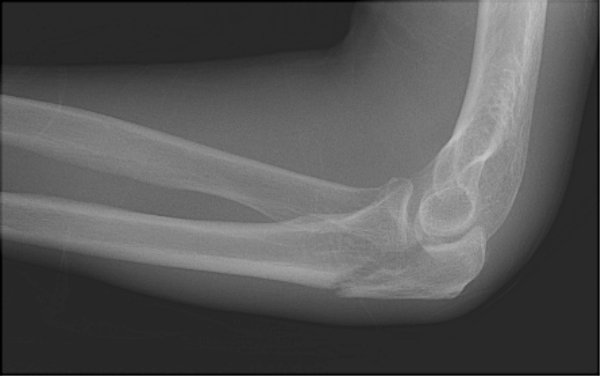
Was an underlying elbow flexion contracture of approximately 15° preoperatively duringĮxamination under anesthesia. The decision was made to proceed with open reduction and internal fixation (ORIF). Contralateral elbow radiographsĬonfirmed that the left olecranon physis was closed ( Figure 2).Ĭontralateral left elbow lateral radiograph demonstrating no olecranon Involving approximately 40% of the joint surface with 1.5-cm displacement ( Figure 1, A and B). Without cortical interruption and bony separation through the olecranon apophysis Initial anteroposterior and lateral radiographs of the right elbowĭemonstrated a persistent olecranon apophysis determined by smooth, rounded edges Compartments of the arm were soft andĬompressible. On physical examination, there was mild swellingĪnd tenderness to palpation of the olecranon along with a palpable gap at the fracture He had no history of injury or pain to the right elbow. Which resulted in immediate pain, swelling, and inability to use the extremity. While playing basketball earlier the same day. Presented to the emergency department with right elbow pain and swelling after a fall Extremely rarely it can mimic a patella cubiti.The patient in this case report was a 16-year-old, healthy, right-hand dominant male who In young patients, one must consider unfused olecranon epiphysis 3. There is usually little differential, especially in adults, and when the clinical presentation is that of trauma to the elbow with pain, swelling and lack of mobility. Occasionally ulnar nerve injury can result in long-term sensory and motor impairment, most marked in the hand. Most of the symptoms relate to prominence of hardware given the little overlying soft tissues 1. Unlike many other intra-articular fractures, olecranon fractures result in relatively little secondary osteoarthritic changes, probably on account of most fractures occurring through a relatively non-articular part of the trochlear groove 1. Union rates with appropriate treatment are very high (~99%) and other than a slight reduction in flexion and extension at the elbow, function is preserved 1,2. Non-operative treatment can be considered for undisplaced fractures or patients with significant medical co-morbidities 2. Presence of fracture of the distal humerusĭue to the unopposed traction of the triceps muscle, these fractures are usually widely displaced and require open reduction and internal fixation (ORIF) 1. Presence of fracture or dislocation of the radial head Presence of fracture of the coronoid process Location, especially whether or not it reaches the articular surfaceĪssociated findings and relevant negatives Radiology reports should not only include whether or not a fracture is present but also comment on: They appear as a lucency usually reaching the trochlear groove articular surface and are, in most cases, displaced. Olecranon fractures are easy to diagnose provided a lateral x-ray of the elbow is obtained. It is important to remember that the ulnar nerve is closely related to the medial aspect of the olecranon and, although not common, nerve injury may complicate these fractures 2. Olecranon fractures occur as the result of one of four mechanisms 2:ĭirect blow (or fall directly on the elbow)įall on outstretched hand with elbow flexedĪvulsion fracture - e.g.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
